Over 15 million Americans currently take a type of heartburn medication known as proton pump inhibitors, or PPIs, to manage their gastroesophageal reflux disease (GERD). However, these medications can be associated with various side effects when used long-term.
Prolonged use of these medicines may be linked to kidney issues, certain cancers, heart concerns, and bone health challenges. Other potential side effects include vitamin B12 deficiency, low magnesium, low calcium levels, and susceptibility to infections.
If you have GERD and are considering alternatives to PPIs, personalized strategies like nutrition and lifestyle modifications may help support symptom management and overall well-being.
This article will discuss common reasons for chronic heartburn, how to explore these conditions, and ways to support your stomach's natural functions.
[signup]
What is GERD
GERD, short for gastroesophageal reflux disease, is associated with frequent acid reflux.
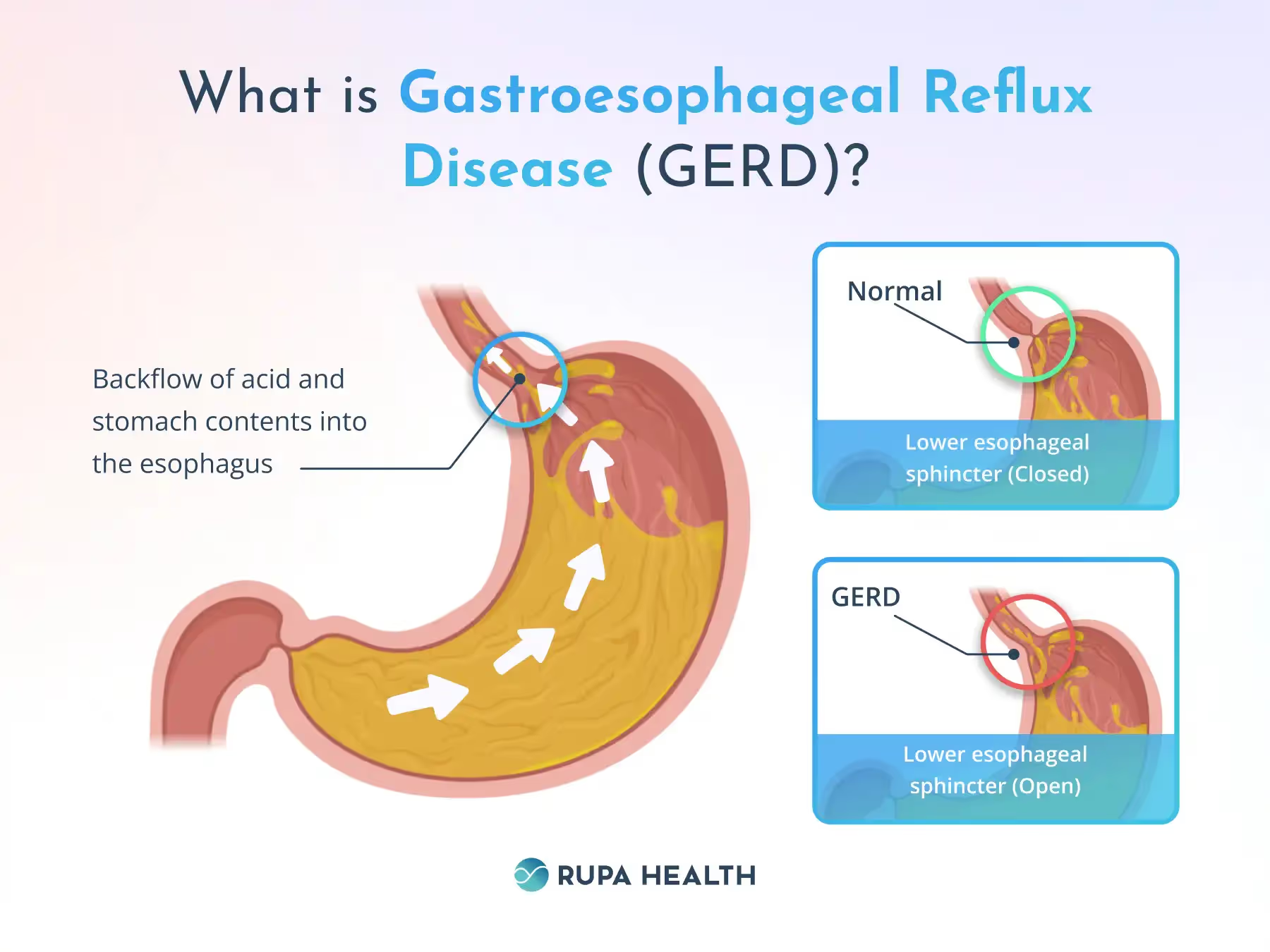
When you swallow, the muscle around the bottom of your esophagus relaxes to allow food and liquid to flow into your stomach. After the food moves down, the sphincter closes behind it. If that muscle relaxes abnormally or weakens, stomach acid can flow back up into your esophagus, causing acid reflux or "heartburn."
Many people experience acid reflux occasionally. But GERD is typically identified if mild acid reflux occurs at least twice a week or moderate to severe acid reflux occurs at least once a week.
GERD Signs & Symptoms
- A burning sensation in your chest (heartburn), usually after eating, which might be worse at night
- Chest discomfort
- Difficulty swallowing
- Regurgitation of food or sour liquid
- Sensation of a lump in your throat
- Chronic cough
- Laryngitis
- New or worsening asthma
- Disrupted sleep
Risk Factors for GERD
- Obesity
- Bulging of the top of the stomach up into the diaphragm (hiatal hernia)
- Pregnancy (changes in hormones and the growing baby can affect digestion)
- Hormonal Imbalances (Estrogen and Progesterone)
- Delayed stomach emptying (this can be for many reasons, including prior viral infection, damage to the vagus nerve, diabetes, and autoimmune disorders)
- Fatty, fried, processed foods (Standard American Diet)
- Smoking
- Eating large meals or eating late at night
- Drinking certain beverages, such as alcohol or coffee
- Taking certain medications, such as aspirin or Motrin
- Low Stomach Acid aka Hypochlorhydria (more on this below)
Acid Reflux and Hypochlorhydria (Low Stomach Acid)
This subject is often overlooked but is important to consider when someone experiences chronic heartburn or GERD symptoms.
Proper stomach acid is needed to break down the foods we ingest. When stomach acid is low, it can leave undigested food particles, slowing down digestion. This may cause a buildup of gas and discomfort, mimicking signs and symptoms of GERD such as indigestion, burping, bloating, and stomach discomfort (or burning after eating).
Common Reasons for Hypochlorhydria
- Age (acid levels may decrease as we get older)
- Long-term use of over-the-counter antacids and proton pump inhibitors (used to manage ulcers and acid reflux)
- Vitamin deficiency (deficiency of zinc or B vitamins may affect stomach acid production)
- H. pylori infections (a common cause of stomach ulcers)
- Chronic Stress
- Gastric Bypass Surgery
If someone doesn't know how to distinguish between low stomach acid symptoms and GERD properly, they may be prescribed a PPI that doesn't address the underlying issue.
But don't worry if you think you have low stomach acid; there is a simple at-home test you can try out.
At-Home Test for Hypochlorhydria
- Mix ¾ tsp of Baking Soda first thing in the morning on an empty stomach
- Set a time and wait 5 mins
- If you create any upper GI gas or burp in the first 5 mins, you may have sufficient stomach acid
- If you do not belch within 5 mins, you might have low stomach acid
Functional Medicine Labs to Explore GERD
While there are no current functional lab tests that directly test for GERD, there are a few standard tests that practitioners use to explore possible underlying factors of GERD.
An unhealthy GI tract, food sensitivities, and female hormonal imbalances are three common conditions that can affect digestion, inflammation, and GERD symptoms.
Comprehensive Stool Test
These stool tests can assess digestive function, dysbiosis (balance of good vs. bad bacteria), intestinal inflammation, and if there is a need for digestive support, including stomach acid (HCL) support, enzymes support, and nutritional changes that the patient may need to consider. This is always one of my go-to tests when someone presents with GERD symptoms (after Hypochlorhydria has been ruled out).
Food Sensitivities
The Standard American Diet is one of the most common reasons for food sensitivities. Food sensitivities can play a role in disrupting the gut microbiome and contribute to symptoms such as gas, bloating, inflammation in the GI tract, and slower digestion leading to Acid Reflux.
Female Hormones
Studies have shown that elevated levels of estrogen and progesterone, either through endogenous or exogenous sources, can be associated with increased gastroesophageal reflux. These hormones are commonly out of balance in post-menopausal women.
Approaches to Support GERD Management
PPIs come with a list of potential side effects, so exploring alternatives may be beneficial for overall health.
Instead, personalized strategies that include nutrition and lifestyle modifications can help individuals with chronic acid reflux find effective symptom management and support recovery.
Functional medicine focuses on the whole body, and we are always asking, "why is this happening?" This means we discuss your diet, daily activities, how you sleep, and many other components of your lifestyle to explore the root of what's causing your symptoms.
Once we identify potential root causes, small steps towards healthy lifestyle modifications can really add up over time. Learning how to cook at home and focus on eating organic whole nutrient-dense foods is important for supporting your gut microbiome, increasing food transit time, reducing inflammation, and managing acid reflux symptoms.
Paleo, Nutritarian, Whole 30, and the Pegan Diet are nutrition plans commonly used by functional medicine practitioners. Each of these plans encourages increasing whole foods consumption and comes with extensive literature and research to support the science behind nutrition and health.
If you have a food sensitivity triggering your symptoms, working with a practitioner to eliminate and slowly reincorporate that food once your GI tract has healed can make a significant difference.
Large meals may also be a challenge for those who experience GERD. Learning how to modify your diet to smaller nutrient-dense meals can help you feel satisfied while giving your stomach and esophagus a much-needed break.
Stress reduction is a crucial component to managing acid reflux. The gut-brain axis is a real thing. If we are constantly in fight or flight, our digestion can be affected. Learning what our stressors are and how to cope with them can significantly impact overall digestive health.
If your practitioner finds your hormones are out of balance, low-dose hormone support may be considered.
Supporting Hypochlorhydria in GERD Management
If you have lower stomach acid and this is contributing to your acid reflux, it's important to address this. Untreated acidity problems can affect the stomach lining or lead to gastric concerns.
In the short term, you can explore ways to support your acid levels to allow the rest of the digestive process to function properly. Natural supplements, including apple cider vinegar and digestive bitters, have been suggested to help support stomach acid balance.
There are also professional-grade supplements that include Pepsin, HCL, and digestive enzymes to assist with digestion. Over time these supplements may help support your stomach in reaching the correct pH levels.
It's essential to work with an Integrative Healthcare Professional when using these supplements to ensure you are getting the proper guidance.
Summary
If you experience GERD and want to explore alternatives to PPIs, nutrition and lifestyle changes can make a significant difference.
Working with an integrative practitioner is highly recommended if you don't know where to start.












%201.svg)







