Seasonal allergies can vary in severity and duration of symptoms based on environmental influences; however, one's allergic propensity may be influenced by factors such as overall inflammatory load, stress, and gastrointestinal health. Due to these connections, approaches that focus on supporting balance within these systems, along with addressing the offending allergic agent, may be beneficial.
[signup]
CC: Fatigue, Seasonal Allergies, Urticaria
Aileen was a 40-year-old female who experienced seasonal allergy symptoms, fatigue, sneezing, itchy and watery eyes, ear and frontal sinus fullness, and occasional topical hives. All of Aileen's symptoms began about one month after moving to the Chicagoland area from Virginia, where she had been living for the past 20 years. Before the relocation, she had never experienced allergies or topical hives and had no known triggers.
The patient had recently gone through 2 years of high stress related to a traumatic divorce and moved cross country with her 5-year-old to live with her parents. On her initial visit, she rated her stress level at 7/10 and was sleeping a solid 8 hours a night. Her energy level was consistently a 5/10 during the day at its best, and she felt tired and unmotivated upon waking.
Additional History
The patient had been a vegetarian for the last eight years while entirely avoiding dairy due to the bloating and gastrointestinal discomfort it caused. Otherwise, her digestion was healthy and regular as long as she continued to avoid her previously identified food sensitivities; an IgG panel had been performed four years earlier due to ongoing constipation, which was resolved by removing the identified foods. She had not challenged the foods for reintroduction since she cut them out four years prior.
She had also previously been supported for adrenal health by a functional medicine doctor years prior when going through a stressful transition at work that left her dealing with fatigue and insomnia. She had a hormone-based IUD implanted around four years ago and only had a full menstrual period every 4-5 months.
She had been taking zinc, vitamin C, and fish oil regularly. Overall, she ate very clean, focusing on beans/legumes at each meal with a hearty portion of vegetables and fruit. She frequently snacked on nuts and plant-based protein shakes between meals.
Lab Work
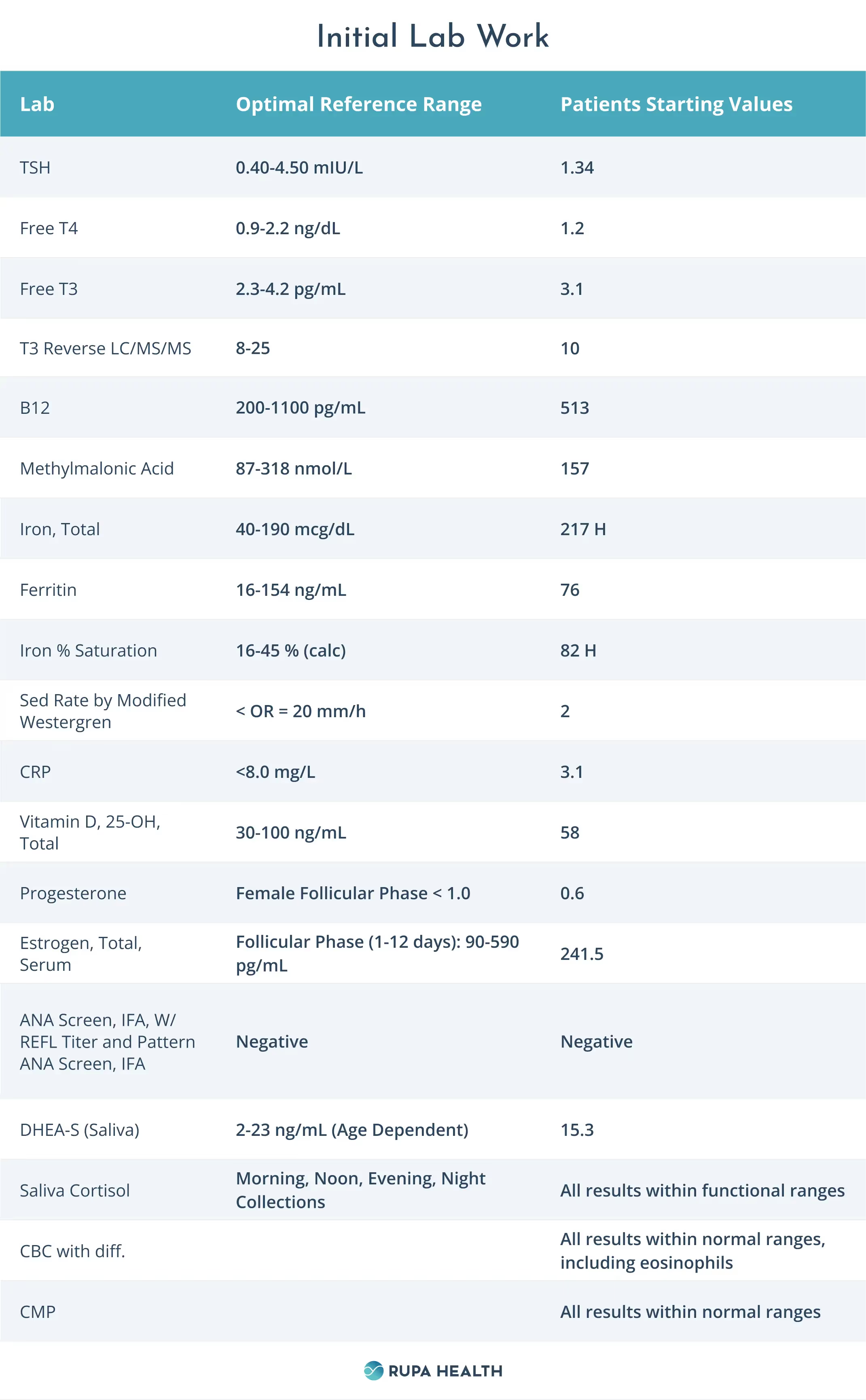
Comprehensive Stool Panel Results
- Fecal Fat Total: low
- Fecal Secretory IgA: mildly elevated at 831
- Short Chain Fatty Acids: low; chiefly n-butyrate concentration low
- Beneficial commensal bacteria: low; chiefly akkermansia muciniphila
Food Sensitivity Panel- 184 foods IgG Results
- Level 1: barley, hops, venison, pistachio/almonds/walnuts/peanuts, lima beans/black beans/lentils/chickpeas/kidney beans
- Level 2: soy beans
Lab Analysis
Aileen's lab work suggests three core issues that may be contributing to her fatigue:
- Secretory IgA: a high level of activity in her gut which may be stemming from or further contributing to identified food intolerances
- High iron levels could contribute to iron overload and may be associated with tiredness and fatigue.
- The patient's vegetarian diet focuses heavily on beans, lentils, legumes, and nuts, and seeds for overall protein intake, all of which may be causing her low-level immune system reactions.
Interventions
- The patient was advised to consider a blood donation to help manage her iron levels.
- Since the seasonal shift seemed to exacerbate her allergic symptoms, and she had no environmental allergy triggers while living in Virginia, she was given Allergena Allergy relief drops specific to the designated zone she was living in. These drops are homeopathic sublingual immunotherapy that may help the body become more tolerant to allergens by providing microdoses of what plants/flora the person is allergic to.
- She was also given Xclear nasal spray and saline packets to use daily.
- Due to the current allergen in the area being grass pollen, she was advised to avoid all fruits/vegetables from the grass family, which included melons, oranges, swiss chard, tomatoes, and watermelon, for 30 days.
- We suggested including high quercetin foods for their potential to support histamine management; raw onions, red apples, red grapes, spinach, capers, cherries, berries, broccoli, asparagus, chili peppers, red leaf lettuce, and green/black tea.
- She was advised to modify her current vitamin C dosage to 1,000 mg morning and night and consider drinking nettle tea 1-3 cups daily with local honey for its potential to support mast cell stabilization.
- She was also given a probiotic nightly and recommended to add acacia powder to her protein shakes to encourage the growth of beneficial commensal bacteria.
- After discussing the potential benefits of collagen and protein, Aileen felt comfortable reintroducing homemade bone broth and fish while beginning to reduce the intake of beans/legumes, and nuts/seeds for 30 days before reintroduction.
Environmental Support
- HEPA air purifier in the bedroom and main room of the house
- Hypoallergenic sheets/pillowcase for bedroom
- Wash clothes and shower after a prolonged period outside
- Washing of all bedding once a week
- Dusting and vacuuming once a week: under the bed, window sills
- Examination of the home for any evidence of mold
- Windows kept closed as much as possible from spring through fall
Follow Up Visit 2 Months Later
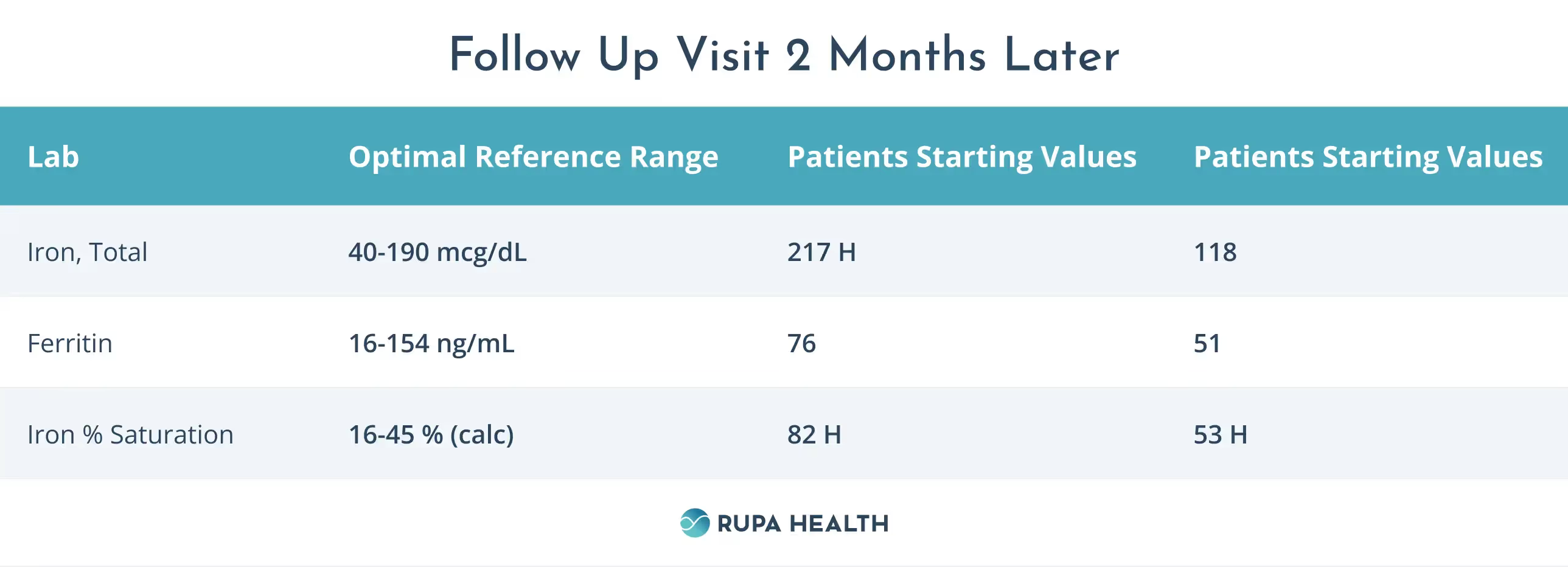
At our follow-up visit two months later, Aileen was feeling much better. Two weeks into her new routine, she noticed a significant improvement in her overall allergy symptoms, with only mild nasal congestion after being outdoors for over 2 hours.
She had 1 round of hives on her mouth, cheek, and hand after cutting up a cantaloupe for her daughter, but no other occurrences.
Her energy level had also improved daily to an 8/10, and she was feeling more refreshed and awake in the morning, no longer needing coffee to get her going. She attributed some of the energy to the animal protein and chose to begin consuming chicken 1-2x a week as well.
Her digestion had always been regular, but she felt her stomach was flatter, and she had lost 5 pounds since our first visit. The patient felt so good that she never reintroduced the nuts/seeds, beans/legumes, or grass family members she removed two months prior.
At this time, the patient was guided on a slow reintroduction process to prevent limiting the body and microbiome of a vast protein and fiber source. She was encouraged to continue with the other diet and supplement additions till summer was over and to stop the allergen drops in October when the season shifts.
Summary
This case highlights the potential impact of the link between gastrointestinal health and allergic responses. Gastrointestinal activity and low bacteria flora may be associated with histamine release and, thus, increase allergy symptoms.
By focusing on whole foods alongside her supplemental allergen drops, Aileen's system may not have such dramatic allergic responses in the future.












%201.svg)







